How Pediatric Trauma Cases Are Handled
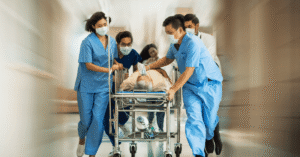
Each second counts in the event that a child suffering from trauma is admitted to the hospital emergency rooms (ER). As pediatric trauma is one of the most common factors that cause morbidity and deaths for children, it’s crucial that emergency facilities be well-organized, have trained staff, and specially-equipped equipment to ensure the best care.
Treatment of trauma in children is very different in comparison to treating trauma for adults because of the physiological, anatomical, and psychological differences that exist among children. This blog focuses on the treatment of trauma patients in emergency rooms. We will discuss the assessment procedures, stabilization techniques as well as the challenges encountered, along with the multidisciplinary approach required to provide life-saving treatment.
What is Pediatric Trauma?
Children are susceptible to trauma from various sources, which include:
- Accidents involving traffic on the road
- Falls
- Injuries from sports
- Burns
- Drowning incidents
- Accidental or non-accidental injuries (child abuse)
Children are distinct from adults in the sense that their bones are more flexible, their head-to-body ratios are greater, and their blood vessels are smaller. That means that any injuries that may seem small initially may lead to grave complications if not addressed promptly. Emergency doctors must alter their methods to take into account the unique characteristics of each patient.
As a leading emergency trauma hospital in Ahmedabad, the facility is equipped with advanced trauma care infrastructure, experienced emergency physicians, and round-the-clock critical care support to manage accidents, severe injuries, and life-threatening emergencies with efficiency and compassion.
The Pediatric Trauma Team
A majority of emergency facilities employ a team-based approach to handling trauma for children. A typical trauma team for children includes:
- Emergency medical professionals: Take over the initial assessment and stabilize.
- Surgery for Trauma: Retake over surgery procedures.
- Specialists in pediatrics: This includes ortho surgeons, neurologists, or intensivists, based on the type of injuries.
- Paramedics and nurses: Trained in the field of pediatric health as well as life support.
- Radiologists: Imagery that is quick as well as assessment.
- Child life experts and social workers offer emotional support for the parents as well as the child.
This approach to collaboration ensures quick decision-making and a thorough approach.
Initial Assessment: The ABCDE Approach
Emergency departments generally comply with the guidelines for trauma assessment set out by Advanced Trauma Life Support (ATLS) or Pediatric Advanced Life Support (PALS). Within the initial few minutes following the arrival of a patient that are vital in the initial minutes following arrival, you should follow the “ABCDE” framework is often utilized:
1. Airway containing Cervical Spine Security
- Children’s airways are smaller and therefore more vulnerable to obstruction.
- In the event of suspicion of injury to the head or neck area, the doctor will assess breathing sounds, airway integrity and then take steps to ensure the cervical spine is protected.
- If airway obstruction is present, the need for intubation could be necessary.
2. Breathing
- Oxygen saturation is kept under observation.
- Heart injuries (such as pneumothorax, flail chest) can be quickly identified.
- If required, oxygen or assisted breathing is provided.
3. Circulation in Hemorrhage Control
- The amount of loss of blood is assessed. The child’s fright is often caused by tiny amounts of blood loss.
- For fluid resuscitation, IV/IO (intraosseous) access is quickly established.
- If there is a serious injury, procedures for massive transfusions could be in the works.
4. Disability (Neurological Status)
- Children’s neurological testing can be conducted with the Glasgow Coma Scale (GCS).
- The signs of head injuries, convulsions or an altered state of mind are analyzed.
Diagnostic Tools in Pediatric Trauma
When the child is stabilized, diagnostic instruments assist in identifying any injuries.
- Ultrasounds and Xrays (FAST examination): Rapid and minimally invasive tests, used to detect fractures as well as internal bleeding.
- CT scans Offer detailed and clear images, especially for cranial and abdominal injuries. They are to be utilized with caution due to radiation exposure.
- Laboratory tests: Blood counts, profile of coagulation, and metabolic panels aid in treatment decision-making.
Emergency doctors face the challenge of maintaining safety and speed, and making decisions regarding imaging that minimize radiation risk and provide crucial diagnosis information. As a trusted emergency trauma hospital in Gota, the facility is equipped with advanced imaging technology and experienced emergency specialists who ensure accurate, fast, and safe diagnosis for effective trauma and emergency care.
Common Types of Pediatric Trauma and ER Management
Trauma to the child can manifest in many ways. Each kind requires a specific procedure in the emergency room. Head traumas and fractures, abdominal trauma, as well as burns, need cautious assessment and quick intervention due to the distinct nature of the physiology of infants. Understanding the common types of trauma in children and the procedures ER teams utilize to manage their care helps highlight the complexity and precision in saving lives.
1. Head Injuries
A larger head for children is a risk factor for head trauma.
- Treatment consists of immediate neurologic evaluations, CT scans when warranted, and monitoring of the intracranial pressure.
- In extreme cases, there may be a need to operate on the nervous system.
2. Chest Trauma
- Though rib fractures may not be uncommon in young children, they may indicate an internal trauma that is serious.
- ER teams search for hemothorax or pneumothorax, which could require the insertion of a chest tube.
3. Abdominal Trauma
- Liver and spleen are quite common among young children.
- Except for bleeding that requires surgical intervention, most cases can be treated without surgery and under attentive observation.
4. Fractures and Orthopedic Injuries
- Children’s bones heal rapidly, but they also need to be checked for alignment in order to prevent growth disruptions.
- In an emergency room in the emergency room, casts or splints are put on, and then followed by ortho treatment.
Pain Management in Pediatric Trauma
Controlling pain is vital for the care of patients in the emergency rooms.
- Pain that is severe can often be treated using either fentanyl intranasally or an intravenous injection of Morphine.
- To induce the purpose of sedation in the procedure, ketamine can be employed.
- Techniques that do not require drugs, such as distraction strategies and child life therapy, as well as having parents in the room are all used.
Communication with Family Members
The most distinctive characteristic of pediatric trauma therapy is the presence of relatives. It is crucial for emergency medical teams to:
- Explain the child’s needs in a clear and compassionate manner.
- When possible, let parents participate in the resuscitation process, since it eases the anxiety.
- Provide guidance and support throughout all stages of caregiving.
Challenges in Pediatric Trauma Care
While there has been improvement in trauma-related care, the emergency room team faces numerous challenges.
- Reducing Anatomy: Complicates managing airways as well as access to intravenous fluids.
- Limitations in physiological reserves: Children’s deterioration develops at a quicker rate than that of adults.
- Emotional Stress: Families and staff might find treatment for kids with serious injuries emotionally difficult.
- Resource Limitations: Pediatric trauma facilities do not exist at all hospitals, and are not available in remote regions.
The Role of Specialized Pediatric Trauma Centers
The general emergency room can help stabilize trauma patients in the pediatric age Pediatric trauma centers that are specialized offer:
- Equipment and facilities for children.
- Pediatric trauma surgeons and experts in critical treatment.
- Pediatric ICUs are specially designed to provide Post-stabilization treatment.
The research shows that children receiving treatment in pediatric trauma centers have higher survival rates and better outcomes in comparison to children treated by an emergency trauma hospital in Ahmedabad.
Post-Trauma Care and Rehabilitation
The emergency treatment is only the initial step to a child’s rehabilitation. Post-trauma care typically covers:
- The Intensive Care Unit is a place for the supervision of serious traumas.
- Rehabilitation and rehabilitation services include physiotherapy, occupational therapy or speech therapy.
- Psychological aid is designed to help parents and their children cope with post-traumatic anxiety.
The long-term monitoring ensures physical healing along with emotional well-being and the return to routine.
Despite the fact that issues like limited resources and stress on the emotional side persist, however, the presence of special pediatric trauma centers, specially trained emergency rooms, and the advancement of treatments keep improving the rate of survival and quality of recovery for children patients. Pediatric trauma care at Lifeline ICU Hospital, It is run by top experts with compassion, professionalism, and the latest medical equipment. The hospital ensures that its young patients are provided with prompt and timely medical attention in critical situations due to the dedicated staff of specialists for children, state-of-the-art emergency services, and 24-hour assistance for critical cases.